Coming Off Weight-Loss Medication: Your 12-Week Transition Timeline
If you are coming off weight-loss medication, the hardest part is usually what happens next: appetite returns, routines drift, and regain can begin before people realise it.
This page gives you a simple educational timeline based on your last dose date, plus a practical maintenance plan for the first 12 weeks after stopping.
This page is designed to help you think ahead, act early, and avoid the common slide that follows stopping.
How to use the tool
Select the medication you have been using.
Enter the date of your last dose.
Read the timeline and follow the focus points for each phase.
You will get a week-by-week guide to what people commonly notice after stopping and what to prioritise next. This tool is educational and does not replace personal medical advice.
Important safety notes (please read)
This tool is educational. It does not replace care from your prescriber.
Speak to your clinician before stopping if any of the following apply
You have type 2 diabetes, use insulin or sulfonylureas, or your glucose control is unstable (stopping can change glycaemic control and may require monitoring/medication adjustment).
You are pregnant, trying to conceive, or breastfeeding.
You have a history of pancreatitis or severe gastrointestinal disease.
You feel unwell, dehydrated, or have persistent vomiting.
Seek urgent help now if you have
Severe abdominal pain (especially with vomiting), fainting, confusion, or signs of severe dehydration.
GLP-1 stopping timeline
Enter your last dose details to see an educational, general timeline of what people often notice and what to focus on next.
Your timeline
Stay up to date
Get occasional updates on coming off weight-loss medication, appetite rebound, maintenance, and practical ways to reduce regain risk after stopping. Enter your details below.
WHY THE FIRST 12 WEEKS MATTER
The effects fade gradually, not overnight.
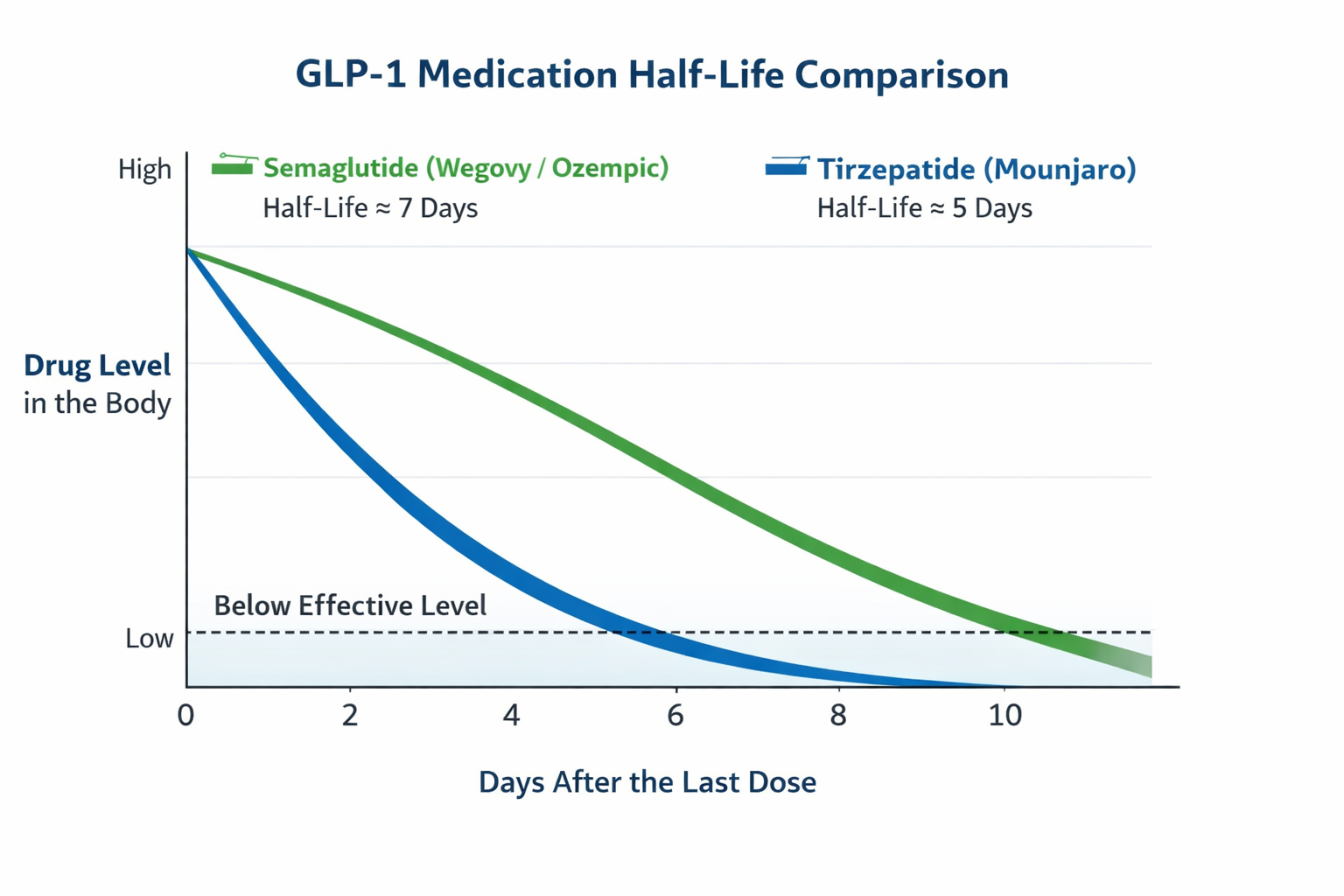
These medications do not disappear all at once. That is why many people feel fine at first, then notice appetite, cravings, and old routines returning later. The tool above is designed to help you anticipate that shift and act early.
WHAT TO EXPECT
A practical week-by-week transition timeline.
Your personalised timeline appears above once you enter your date. This is the general pattern many people recognise after stopping.
In clinical trials, many participants regained a substantial proportion of lost weight after stopping GLP-1 therapy.
In the STEP 1 extension, people regained about two-thirds of prior weight loss one year after stopping semaglutide (on average), alongside reversal toward baseline of several cardiometabolic improvements. [1]
In SURMOUNT-4, participants who stopped tirzepatide and switched to placebo regained significant weight compared with those who continued. [2]
Takeaway: obesity and appetite regulation behave like a chronic biology + environment problem. If you’re stopping, your plan needs to be at least as structured as the medication was.
THE BIG REALITY
Regain risk is real and it’s not a moral failure.
MAINTENANCE PLAN
A simple, effective, and non-obsessive approach to use as a default week.
WHO THIS TOOL IS FOR
FAQ
The practical questions — answered clearly.
-
Some people stop abruptly; others step down. The right approach depends on why you’re stopping (side effects, cost, pregnancy planning, response, diabetes control). If you have diabetes or are on other glucose-lowering meds, discuss a plan with your clinician. [3]
-
Because these drugs have long half-lives, appetite often returns gradually over weeks, not overnight. Semaglutide is ~1 week half-life; tirzepatide ~5 days. [4]
-
Not inevitable, but risk is higher if routine slips. Trials show substantial regain after withdrawal for many people, which is why a maintenance plan matters. [1]
-
For most people: meal structure (planned meals, less grazing) + protein anchors + strength training. If you only do one thing, build a repeatable week.
-
No. Appetite drive is biology plus environment. This is exactly why people struggle after stopping, and why “just try harder” is a weak strategy.
-
Persistent vomiting, severe abdominal pain, dehydration, or escalating symptoms need medical review. If symptoms are mild, focus on hydration and gentle foods, then get clinician advice if they persist.
ABOUT DR DAN
Practical support for the gap between stopping and stabilising.

I work in NHS emergency medicine and private practice, with a particular interest in what happens after the prescription: appetite rebound, habit drift, weight maintenance, and the gap between a plan on paper and real life.
This page is designed to give people a calmer, more practical first 12 weeks after stopping.
NHS A&E doctor
Private work in deprescribing and metabolic health
Public educator focused on practical behaviour change
NEED A MORE STRUCTURED PLAN FOR THE FIRST 12 WEEKS?
If you are about to stop, have already stopped, or feel appetite and weight drifting after stopping, book a consultation. I help people build a realistic transition plan that covers food, training, routine, tracking, and follow-up.
Clinical appointments are provided by CQC-registered Sutton Medical Consulting
This is not for urgent symptoms. If you have severe abdominal pain, persistent vomiting, dehydration, fainting, or concerns about diabetes control, seek medical advice urgently.
References
Wilding JPH, Batterham RL, Davies M, Van Gaal LF, Kandler K, Konakli K, Lingvay I, McGowan BM, Oral TK, Rosenstock J, Wadden TA, Wharton S, Yokote K, Kushner RF; STEP 1 Study Group. Weight regain and cardiometabolic effects after withdrawal of semaglutide: The STEP 1 trial extension. Diabetes Obes Metab. 2022 Aug;24(8):1553-1564. doi: 10.1111/dom.14725. Epub 2022 May 19. PMID: 35441470; PMCID: PMC9542252. https://pmc.ncbi.nlm.nih.gov/articles/PMC9542252
Aronne LJ, Sattar N, Horn DB, et al. Continued Treatment With Tirzepatide for Maintenance of Weight Reduction in Adults With Obesity: The SURMOUNT-4 Randomized Clinical Trial. JAMA. 2024;331(1):38–48. doi:10.1001/jama.2023.24945 https://jamanetwork.com/journals/jama/fullarticle/2812936
FDA prescribing information https://www.accessdata.fda.gov/drugsatfda_docs/label/2025/215256s024lbl.pdf
FDA prescribing information https://www.accessdata.fda.gov/drugsatfda_docs/label/2021/215256s000lbl.pdf